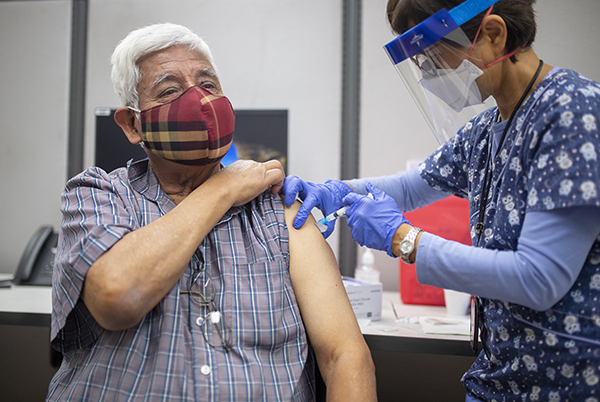
Aftereffects of COVID-19 could be worse, experts say
By Marie Y. Lemelle
Contributing Writer
Think the worse is over after surviving COVID-19? Think again.
National and global studies reveal that the persistent aftereffects of mild to severe COVID-19 has stumped medical professionals, scientists and researchers who find out that new symptoms are causing survivors to suffer from persistent aftereffects from extreme fatigue problems, shortness of breath, to brain fog, depression and even psychotic episodes.
The USC Center for Health Journalism reports the suffering isn’t limited to the most severe cases of COVID-19. The syndrome known as long COVID or long hauler is a persistent debilitating set of symptoms that is affecting thousands of Americans and counting.
“Earlier in the pandemic, we first began to hear about people called long haulers who suffered lingering symptoms of COVID,” said Michelle Levander the founding director of the USC Center for Health Journalism. “These days, new studies are emerging that are starting to tell us much more about how prevalent these conditions might become.
The scientific findings are sure of one thing: full recovery may not be possible for all COVID survivors.
“We first started seeing long COVID emerging in our cohort of patients that we were managing around late April, early May of 2020,” said David Putrino, the director of rehabilitation innovation for the Mt. Sinai Health System in New York City and a physical therapist with a Ph.D. in neuroscience who cared extensively for long COVID patients since the pandemic began.
He said it was first seen in a large group of people with acute COVID symptoms, who were being managing with telehealth to keep them out of the hospital, because at the time beds were not available.
In that group, Putrino said, about 10% of the patients weren’t getting better.
“They were having persistent symptoms such as shortness of breath, headaches and chest pain, and then they were developing new symptoms like extreme fatigue exercise intolerance, cognitive issues, you know, difficulties such as short-term memory loss, difficulty concentrating, issues finding the right words problems with executive function and emotional control,” Putrino added.
The medical community started to suspect that what they were seeing was a post viral syndrome, which is quite common through history with viral outbreaks that typically are followed by a number of individuals who find it difficult to shake persistent symptoms.
“As we’ve worked on cataloguing these symptoms, which are very diverse, highly debilitating and affect the entire body, we are tracking around 60 or more symptoms indicating distinct individual symptoms and started slowly to get a handle on best practices for managing what could be one of many syndromes,” Putrino said. “We’re starting to unlock those medical mysteries.”
The experts agree that it is rare to talk to someone who only has one symptom.
“It’s multiple symptoms that interact with each other,” said Pam Belluck, a health and science writer for the New York Times. “I’ve seen studies and talked to some patients recently who seem to suggest that symptoms can come in clusters.
“People get over one set of symptoms and think they’re OK and then a couple months later something else starts to happen. It is very complex,” she added.
Depending on where you are in the country, the numbers reported are from 10% to 35% of people who have had an acute COVID-19 infection who will get symptoms consistent with long COVID.
National Institute of Allergy and Infectious Diseases Director Dr. Anthony S. Fauci, recently spoke about post-acute sequelae of COVID. Fauci warned of key signs to look out for such as extreme fatigue, muscle aches, temperature dysregulation and brain fog. Finger tremors and seizures and neurological symptoms can sometimes accompany brain fog.
“This is a real phenomenon,” Fauci said in a TV interview. “I, myself, personally, am dealing and helping a number of people who have a post-acute COVID-19 syndrome. They are virologically OK.
“The virus is no longer identified in them, but they have persistence of symptoms that can be debilitating. It can be really quite disturbing.”
According to the National Institutes of Health, “The epidemiology is not fully characterized, and it will need to be expanded in order to identify and help vulnerable groups of people. The full clinical spectrum of post-acute COVID-19 is not yet known, nor the reasons why the symptoms manifest so differently in individuals”
“Post-acute sequelae of COVID are basically anyone who’s having a symptom, after their initial acute COVID infection falls into this big overarching umbrella,” Putrino said. “Post-acute COVID literature states up to 70% to 80% of individuals who are hospitalized with COVID will end up with one or more persistent symptoms”
Putrino talks about his collaboration with the Center for Post-COVID Care Director Dr. Zijlan Chen.
“We use a chart to track when someone shows up to the center for post-COVID care with persistent symptoms,” Putrino said. “Dr. Chen can look at a blood test or a scan and see a proximate cause for those symptoms, such as shortness of breath and he sees extensive lung damage. The patient will be sent to pulmonary rehab.”
Dr Chen manages individuals who have a very clear medical cause for their persistent symptoms. Individuals who have medically unexplained physical symptoms are the people that are typically classified as long COVID.
Unfortunately, a lot of symptoms that patients have presented to their medical professionals are being dismissed and told its psychosomatic, mainly because the physician does not know what to do.
“I would say that it’s been this horribly fascinating thing to watch,” Putrino said. “We learned and are aware of health disparities. I have been watching a health disparity emerge in front of my eyes and that’s been distressing and frustrating.”
He goes on to state about how health disparities continue.
“It doesn’t surprise me at all, from a pragmatic point of view that it’s only white women who are getting this condition because I’m fairly certain that a Black woman who walks into a hospital system who is used to being discriminated against is going to suffer,” he said. “We are concerned that the medical journals are not letting us publish on the cases that are most likely to help minorities and most likely be people who are living in low socioeconomic status communities.”
Due to the lack of resources for testing in low-income communities and communities of color, individuals who never had the COVID test and now are experiencing symptoms of long COVID are going to be at a double disadvantage to be treated, he said.
Marie Y. Lemelle, is the founder of www.platinumstarpr.com and a film producer. She can be reached at MarieLemelle@platinumstarpr.com. Follow her on Instagram @platinumstarpr.