COVID-19 impacts the pregnancy experience
Rx REPORT
By Marie Y. Lemelle
Contributing Writer
With record-breaking unemployment rates because of the coronavirus, it’s not surprising that couples are delaying plans to have a baby. While celebrities seem to be experiencing a baby boom, birth rates are actually on a decline.
For the majority of the real world, mounting debt, zero savings, food insecurities, health care costs, the election, natural disasters and the lack of affordable housing and child care contribute to the decision not to start a family.
The Centers of Disease Control and Prevention reports that births in 2019 decreased by 1% when compared to 2018. Until the U.S. Census 2020 count is finalized, it is unsure how COVID-19 will have a lasting effect on pregnancies and births.
According to several studies, including by the U.S. Department of Agriculture, the cost of raising a child until 17 years old can be upwards of $200,000 depending on where you live and other factors.
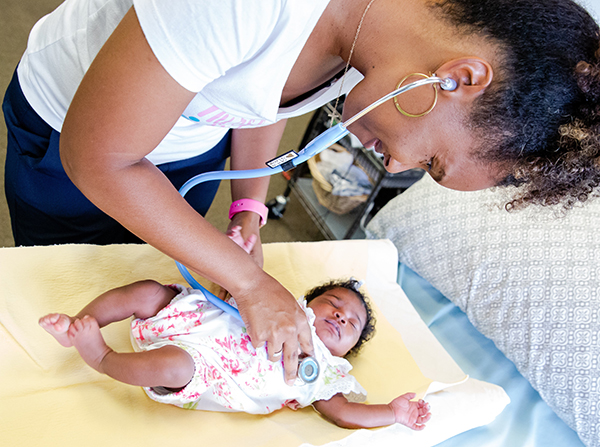
For those who are expecting a new addition to the family in spite of COVID-19 and other obstacles, it’s people like family nurse practitioner Nikki Hunter Greenaway who give expectant parents hope by providing prenatal education and postpartum and women’s health home visits. Greenaway, a wife, and mother of three, is an international board-certified lactation consultant and health strategist who thrives in maternal-child health, reproductive justice, and activism.
As the founder and medical director of Bloom Maternal Health mobile clinic and Nurse Nikki Health Consulting in New Orleans, she works with pregnant and postpartum woman whose recurring theme since COVID-19 shut down the world is they feel alone. To observe October’s World Mental Health Awareness and National Depression Screening, Greenaway highlights some of the stressors felt by perinatal families and how we can provide support to mothers.
ML: What was your inspiration to open your mobile clinic and do the work you do?
NHG: Eight years ago, I was diagnosed with postpartum depression. My health provider told me to find a therapist and support group. What my provider didn’t know is that I barely made it to that six-week check-up due to physical and mental pain. I was really confused and hurt by the lack of support that mothers received after giving birth. My practice, Bloom Maternal Health, is my therapy. People may not realize that home visits for postpartum families is how our ancestors practiced midwifery and how the rest of the world values the postpartum period. When the baby is healthy, and mama is healing, both are thriving.
ML: How does the feeling of alone relate to the pandemic with pregnant and postpartum women?
NHG: Giving birth and recovering can be a lonely experience when you are experiencing emotions, pain and fatigue. The pandemic adds another level of loneliness because of social distancing. Parents are left without physical support and caring for a home, new baby, and recovering from delivery all alone.
ML: What are coping mechanisms for pregnant women?
NHG: I encourage moms to use technology, such as Zoom for virtual support with groups, family and friends. Go outside as often as possible to get fresh air and Vitamin D because it’s a mood booster. I also encourage mothers to continue to provide the essentials for a healthy body: take your prenatal vitals, hydrate and nourish your body.
ML: What are the many stressors felt by perinatal families in the early stages of pregnancy and post birth?
NHG: Often perinatal families wonder if they will be good parents. To address that concern, new parents take classes, read books and join groups but many of those practices have changed since the pandemic. We’ve had to reimagine how parents receive perinatal information. Many mothers are concerned about their health due to the lack of in-person prenatal visits. They don’t get the opportunity to hear fetal heart tones or get their blood pressure assessed. Similarly, in the postpartum period, mothers wonder if they are healing properly.
ML: How can women be supported?
NHG: Who will mother the mother? My goal is to bridge the gap between hospital and community care. Many women fall off the radar and only reappear when in crisis mode. Supported mothers will thrive with the help of others. The pandemic highlighted the fact that the health system does a horrible job of supporting mothers, which is reflected in our dismal maternal morbidity and mortality rates.
ML: How does COVID-19 cause perinatal stressors?
NHG: The current state of prenatal care is virtual obstetrician (OB) visits and classes. No one was prepared to implement virtual prenatal care. How would the labs be handled? How do we manage our high-risk clients? What if the client cannot connect to the internet? Many of my OB colleagues said their phones were ringing off the hook because patients had questions that no one had answers to. Prenatal care was not designed to be delivered virtually. The ramifications scared everyone but no one as much as the pregnant mother.
Parents, especially those that are high-risk, must access hospital services to receive care. Many times, they feel rushed and not heard because doctors and nurses try to move everyone along as quickly as possible to avoid prolonged exposure to a hospital environment. Hospital stays were shorter and less personable. Families could no longer sit in the waiting room for the arrival of new family member. This is not how families pictured their deliveries.
My expectant clients were excited about learning how to swaddle a baby, change a diaper and prepare for breastfeeding, which we provide at the New Orleans Breastfeeding Center. The pandemic warranted the need to cancel classes and childbirth educators didn’t know how to virtually educate families. Many families expressed concerns about not being prepared for parenthood.
Postpartum recovery was another challenge. Prior to COVID-19, providers in Louisiana estimated that about 60% of women returned for their in-person postpartum check-up. Due to COVID-19 restrictions, the American College of Obstetricians and Gynecologists advised OBs to offer virtual postpartum visits to low-risk mothers. The numbers may have decreased, especially for families in marginalized communities.
Low-risk families decided to reach out to local midwives who provide birthing options at a birthing center or in the client’s home. The care is personalized and in-person. I continued to provide home care after equipping myself with personal protective equipment and Lysol. Childbirth educators created virtual courses that relied on parents having a supply list of baby items and participating in a virtual group setting. My hope is that virtual perinatal care is not the new normal.
Marie Y. Lemelle, is the founder of www.platinumstarpr.com and a film producer. She can be reached at MarieLemelle@platinumstarpr.com. Follow her on Instagram @platinumstarpr.





